Coarctation Of Aorta
It is a type of disorder that relates to narrowing down of aorta, the large vessel of blood that emerges from the heart and delivers blood rich oxygen to other parts of the body. Due to coarctation, the heart has to pump harder to push blood through the narrow aorta. The coarctation blocks the normal flow of blood to the body. The narrowing down of aorta is usually spotted when the arteries move towards the upper body. If this condition is too severe in nature, sufficient blood may not be able to reach the lower parts of the body. Because of intense pumping, the heart’s wall thickens while the muscles of the heart weaken. If aorta does not widen, the heart might get so weak that it could lead to a heart failure too.
The coarctation of aorta does not occur alone, but is accompanied with some other defects of the heart. It is a congenital defect that is present at the time of birth, but it may not be detected until later in life. Some children might overcome the effects of the disease and grow normally while some others may have to undergo surgeries for repair and take medical treatment to lessen the symptoms and normalise the flow of blood through the body. This defect constitutes 5-8% of the heart defects that are congenital.
Subclavian Flap Aortoplasty For Aorta
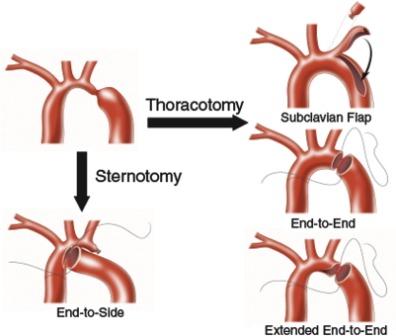
A portion of the blood vessel that delivers blood to your left arm (left subclavian artery), might be used to expand the narrowed area of the aorta.
Top Doctors In India For Subclavian Flap Aortoplasty For Aorta

Dr. Murtaza Ahmad Chishti
35 years of experience , Gurugram, Delhi/NCR, India

Dr. Surinder Bazaz
40 years of experience , Gurugram, Delhi/NCR, India

Dr. Vinayak Aggarwal
24 years of experience , Gurugram, Delhi/NCR, India

Dr. Vijay Kumar Chopra
42 years of experience , Gurugram, Delhi/NCR, India
Top Hospitals In India For Subclavian Flap Aortoplasty For Aorta
Jaypee Hospital, Noida
Established in : 2013
BLK Super speciality hospital, New Delhi
Established in : 1959
Artemis Hospital, Gurugram
Established in : 2007
Max Super Speciality Hospital, Saket, New Delhi
Established in : 2006






