Cosmetic Surgery & Plastic Surgery
Cosmetic surgery is a unique discipline of medicine focused on enhancing appearance through surgical and medical techniques. Cosmetic surgery can be performed on all areas of the head, neck and body. Because treated areas function properly but lack aesthetic appeal, cosmetic surgery is elective.
Cosmetic surgery procedures include:-
- Breast Enhancement: Augmentation, Lift, Reduction.
- Facial Contouring: Rhinoplasty, Chin, or Cheek Enhancement.
- Facial Rejuvenation: Facelift, Eyelid Lift, Neck Lift, Brow Lift.
- Body Contouring: Tummy Tuck, Liposuction, Gynecomastia Treatment.
- Skin Rejuvenation: Laser Resurfacing, Filler Treatments.
Plastic surgery is defined as a surgical speciality dedicated to the reconstruction of facial and body defects due to birth disorders, trauma, burns, and disease. Plastic surgery is intended to correct dysfunctional areas of the body and is reconstructive in nature.
Plastic surgery procedures include:-
- Breast Reconstruction
- Burn Repair Surgery
- Congenital Defect Repair: Cleft Palate, Extremity Defect Repair
- Lower Extremity Reconstruction
- Hand Surgery
- Scar Revision Surgery
Skin grafting
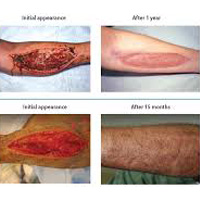
A skin graft is used to permanently replace damaged or missing skin or to provide a temporary wound covering. This covering is necessary because the skin protects the body from fluid loss, aids in temperature regulation, and helps prevent disease-causing bacteria or viruses from entering the body. Skin that is damaged extensively by burns or non-healing wounds can compromise the health and well-being of the patient.
Injuries treated with skin grafts:
Skin grafting is sometimes done as part of elective plastic surgery procedures, but its most extensive use is in the treatment of burns. For first or second-degree burns, skin grafting is generally not required, as these burns usually heal with little or no scarring. With third-degree burns, however, the skin is destroyed to its full depth, in addition to the damage done to underlying tissues. People who suffer third-degree burns often require skin grafting.
Wounds such as third-degree burns must be covered as quickly as possible to prevent infection or loss of fluid. Wounds that are left to heal on their own can contract, often resulting in serious scarring; if the wound is large enough, the scar can actually prevent movement of limbs. Non-healing wounds, such as diabetic ulcers, venous ulcers, or pressure sores, can be treated with skin grafts to prevent infection and further progression of the wounded area.
Types of Skin Grafts:
Split-level thickness grafts:
These grafts comprise two layers of the skin, the epidermis, and dermis. These layers are taken from the area where the skin is healthy.
Full-Thickness Grafts:
These grafts comprise the muscles and the blood vessels in addition to the top of the two layers of the skin from the donor site. It is used for small wounds on highly visible parts of the body such as the face. It blends well with the surrounding skin and usually grows with the other skin.
Composite Grafts:
These grafts comprise skin and underlying cartilage or other tissue. It is used to reconstruct nasal rim defects.
Top Doctors In India For Skin grafting

Dr. Shilpi Bhadani
14 years of experience , Gurugram, Delhi/NCR, India

Dr. Anshu Mishra
7 years of experience , New Delhi, Delhi/NCR, India

Dr. Lokesh Kumar
30 years of experience , New Delhi, Delhi/NCR, India

Dr. Anil Kumar Murarka
32 years of experience , New Delhi, Delhi/NCR, India
Top Hospitals In India For Skin grafting
BLK Super speciality hospital, New Delhi
Established in : 1959
Artemis Hospital, Gurugram
Established in : 2007
Fortis Memorial Research Institute, Gurgaon, Gurugram
Established in : 2013
Medanta - The Medicity, Gurugram
Established in : 2009






