Cosmetic Surgery & Plastic Surgery
Cosmetic surgery is a unique discipline of medicine focused on enhancing appearance through surgical and medical techniques. Cosmetic surgery can be performed on all areas of the head, neck and body. Because treated areas function properly but lack aesthetic appeal, cosmetic surgery is elective.
Cosmetic surgery procedures include:-
- Breast Enhancement: Augmentation, Lift, Reduction.
- Facial Contouring: Rhinoplasty, Chin, or Cheek Enhancement.
- Facial Rejuvenation: Facelift, Eyelid Lift, Neck Lift, Brow Lift.
- Body Contouring: Tummy Tuck, Liposuction, Gynecomastia Treatment.
- Skin Rejuvenation: Laser Resurfacing, Filler Treatments.
Plastic surgery is defined as a surgical speciality dedicated to the reconstruction of facial and body defects due to birth disorders, trauma, burns, and disease. Plastic surgery is intended to correct dysfunctional areas of the body and is reconstructive in nature.
Plastic surgery procedures include:-
- Breast Reconstruction
- Burn Repair Surgery
- Congenital Defect Repair: Cleft Palate, Extremity Defect Repair
- Lower Extremity Reconstruction
- Hand Surgery
- Scar Revision Surgery
Reconstructive Burn & Scar Surgery
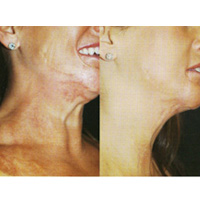
Surgery will not be able to remove a patient’s burn scars entirely, but it will help improve basic functions and make scars less noticeable. Scarring can limit the normal motion of the neck, shoulder, hands, or legs. Often surgery to help release this contracture can help a patient regain range of motion. Facial scarring that leads to problems with the eyelids, lips, nose, or hair loss can also be helped with reconstructive burn surgery. Scars that are abnormally thick, wide, or discoloured might also be improved by a variety of operative and non-operative methods.
What are the options for reconstructive burn treatment?
Non-operative therapies might involve scar massage, application of pressure garments, or other topical therapies. There are a variety of ways to close these wounds depending on a patient’s needs. Skin grafts, skin rearrangement (sometimes called Z-plasty), and more complex skin donor flaps could be used, depending on the location of the scar and a patient’s personal goals. Most minor procedures are performed as outpatient surgery, but the larger grafts and flaps would likely require an inpatient stay. Tissue expansion can also be used as an alternative to skin grafting. Excellent results are commonly attained when performing tissue expansion to regions of the face, neck, arms, hands, and legs.
After Surgery
Following post-surgery instructions are important to heal and obtain the best possible outcome, both in terms of function and physical appearance. You will have to follow up appointments so your surgeon can assess your long-term results and answer any questions or concerns you may have. Since a variety of procedures can be performed, your individual postoperative instructions may vary. In general, skin grafts require kind of "bolster" dressing to keep them in place for 3-5 days without any movement of the skin graft. The bolster helps the skin graft “stick” to the wound and begins to heal. Smaller operations (scar revisions, Z-plasties) might require only a small, soft dressing afterwards. After scar releases on the hand, your surgeon may place you in a larger dressing that incorporates a plaster splint for support after surgery. Additional physical therapy or occupational therapy may be required in the weeks and months following surgery to ensure a complete recovery of function. This may involve splints or casts, as well as exercises you perform at your treatment visits and on your own at home. Your surgeon and therapists will work together to develop the plan that is best for you.
Top Doctors In India For Reconstructive Burn & Scar Surgery

Dr. Shilpi Bhadani
14 years of experience , Gurugram, Delhi/NCR, India

Dr. Anshu Mishra
7 years of experience , New Delhi, Delhi/NCR, India

Dr. Lokesh Kumar
30 years of experience , New Delhi, Delhi/NCR, India

Dr. Anil Kumar Murarka
32 years of experience , New Delhi, Delhi/NCR, India
Top Hospitals In India For Reconstructive Burn & Scar Surgery
BLK Super speciality hospital, New Delhi
Established in : 1959
Artemis Hospital, Gurugram
Established in : 2007
Fortis Memorial Research Institute, Gurgaon, Gurugram
Established in : 2013
Medanta - The Medicity, Gurugram
Established in : 2009






